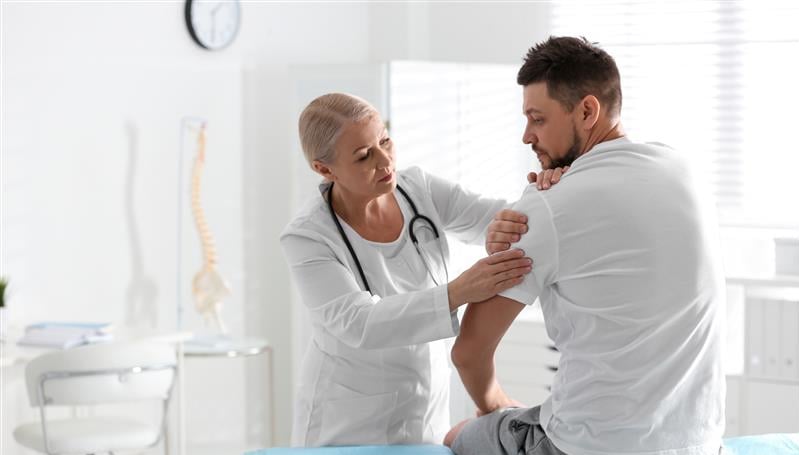
Bedside Manner: What Young Physicians Might Be Missing
Has bedside manners become a lost art? Have the demands of modern medicine made it difficult for young physicians to master the most basic patient-centered care?
A 2013 study by Johns Hopkins University indicated new physicians may need some additional training in this area, at least.
The researchers observed first-year internal medicine interns as they interacted with patients, to see if they employed five strategies of etiquette-based communication:
- Introducing themselves to patients
- Explaining their role
- Touching patients
- Sitting down with the patient for a conversation
- Asking open-ended questions, like “How are you?”
While the young doctors used some strategies more than others, the researchers found that they used all five strategies just 4 percent of the time. The study authors noted that the interns were probably not being rude intentionally, but they may have overlooked the need to build a connection with the patient when concentrating on the medical situation at hand.
Yet, such inefficient communication and lack of connection can have consequences.
Connect with locum tenens job opportunities across the U.S.
The Importance of Good Bedside Manners
Whether a new physician learns from a mentor, from medical school, or just from experience, an effective bedside manner is a key part of his or her job as a physician. It can help establish connections with patients that can lead to better patient compliance and better patient outcomes.
“Bedside manner is crucial to the doctor-patient relationship and goes a long way to help successful healing,” said Clifford Jeng, MD, medical director of The Institute for Foot and Ankle Reconstruction at Mercy Medical Center in Baltimore.
Some studies have shown that a physician’s bedside manner can make significant differences in a patient’s health, helping them to lose weight, lower their blood pressure, and even manage pain. Patient satisfaction scores are also directly affected by whether or not the person feels a connection to their physician.
No matter what your age or experience level in medicine, it may help to review your bedside approach to ensure you are making the most of every patient encounter.
Start From the Beginning
You know that old adage, that you only get one chance to make a first impression? The moment you walk through the door, the patient is assessing you.
“A welcoming smile along with a simple ‘Good morning,’ can go a long way toward building a foundation of mutual respect,” said John-Paul H. Rue, MD, orthopedic sports medicine surgeon with Mercy Medical Center in Baltimore.
If you seem distant or remote, even if you’re just thinking about something, your patient will pick up on that. If you remain standing, rather than sitting down, your patient may feel at a disadvantage. And it could put a damper on your relationship.
“There could be some very correctable things that doctors don’t even know they’re doing,” said Jason Atienza, MD, Orlando Health’s corporate medical director of rehabilitation medicine.
Understand the Patient’s Perspective
Physicians at Orlando Health can participate in a program designed to help them assess and improve their bedside manner, and many have found it helpful.
Atienza described one scenario in which a participating physician received negative feedback from patients because he tended to sit with his arms crossed. He was surprised to learn that people didn’t respond favorably to him because he was concentrating on how to help them and didn’t realize how his presentation affected them. A couple of simple changes later, the physician’s patient experience scores improved dramatically.
What If You’re Not Sure How You Come Across to a Patient?
Atienza suggests having someone video you during a patient encounter. “Talk about an eye-opener, when you see yourself, on camera,” he said.
Five Evidence-Based Tips for Connecting with Patients
A study by Donna M. Zulman, MD, MS, and colleagues, published in January 2020in JAMA, uncovered evidence-based practices that promote clinician presence during patient encounters, using a systematic review of the literature.
The authors issued five recommendations to promote better connections between physicians and patients:
1. Prepare with intention. Take a few moments in advance to get ready to see your patient.
2. Listen completely and intently. Use your body to convey that you’re paying close attention, by sitting down, unfolding your arms and making eye contact.
3. Agree on what matters most. Together, you and your patients can develop shared priorities.
4. Connect with your patient’s story. Consider your patient’s perspective and how their personal circumstances affect their health.
5. Explore emotional cues. Are you watching for the unspoken signs that give insight into how your patient is feeling? Notice and validate your patient’s emotions.
“It’s actually not that difficult,” said Nicholas Jones, MD, a plastic surgeon who practices in Atlanta. “Just put yourself in your patient’s shoes. How would you like to be treated? Remembering that the patients are in a very vulnerable position.”
Advice For Young Physicians, and Others Who Need a Refresher
Every clinician can have a bad day—or just a really hectic day. Those are the times when it can be hard to remember all the small details that help you be truly patient-centered.

“I tell my students that even on your busiest day when you are not happy or you are burnt out, that is the day when your bedside manners are at test,” said Atif Zafar, MD, medical director of the UNM Stroke Program and author of Why Doctors Need to Be Leaders.
It's about cultivating empathy for your patients and approaching them with the genuine intention to serve them, said Zafar. Imagine the kind of care that you’d want your mother, father, or another family member to get, and strive to provide that kind of service.
Empathy really is key, agreed Rue.
“There are many times when a patient will come to see me with a concern, but really what they are looking for is someone to hear them out and listen to their concerns,” Rue said. ‘Oftentimes, even without solving the problem, just offering an empathetic ear to listen and provide some reassurance is all that is needed.”
You may feel rushed, or you may feel you don’t have time. But a good bedside manner is too important to abandon striving toward. Maintaining good physician-patient relationships is not only important for your patients’ health; it also contributes to your practice’s bottom line.
“You can be flawless with the ‘book’ part of medicine, making the right diagnosis and treatment, but if the patient can’t relate to you and doesn’t trust you, they may go looking for another doctor,” said Jeng.
Related:
Building Patient Trust with Effective Doctor-Patient Communication
The Average Time Doctors Spend with Patients
AMN Healthcare has locum tenens jobs in a variety of specialties that can advance your medical career, including part-time and full-time assignments.
Search Physician Jobs in Your Specialty Now
Additional Locum Tenens Resources
While you continue your physician job search for the perfect position, AMN Healthcare provides great resources to keep your career moving in the right direction. Begin the application process now, and then learn more about how AMN Healthcare can help you keep your career on the move.
- EAP: Our locum tenens gain access to a valuable set of Employee Assistance Program benefits.
- Physician Jobs by Specialty: Explore physician jobs and learn about hourly salaries and the benefits of working locum tenens.
- Search All Physician Jobs: Uncover new possibilities in your physician career by exploring both short and long-term options and permanent choices.
- Candidate Benefits: AMN Healthcare takes care of our locum tenens with a variety of amazing benefits. Check out what's in store for our locums.
- Physician Licensing: Check out how we help move your career in amazing directions, both professionally and geographically.
- More Physician Resources: Use the content here to learn everything you need to know about our physician recruitment process.