
DEI Awareness: COVID-19 and Healthcare Disparities
According to the World Health Organization, “health” is a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity. Social well-being is often an overlooked aspect of health and wellness.
On April 7, 2020, Dr. Anthony Fauci, Director of the National Institute of Allergy and Infectious Diseases stated, “Health disparities have always existed for the African American community, but this crisis [COVID19] is shining a bright light on how unacceptable that is. It’s not that [Black Americans] are getting infected more often, it is that when they do get infected, their underlying medical conditions are what lead to the ICU and death… and when all of this is over – there will still be Healthcare disparities, which we will need to address in the African American community.”
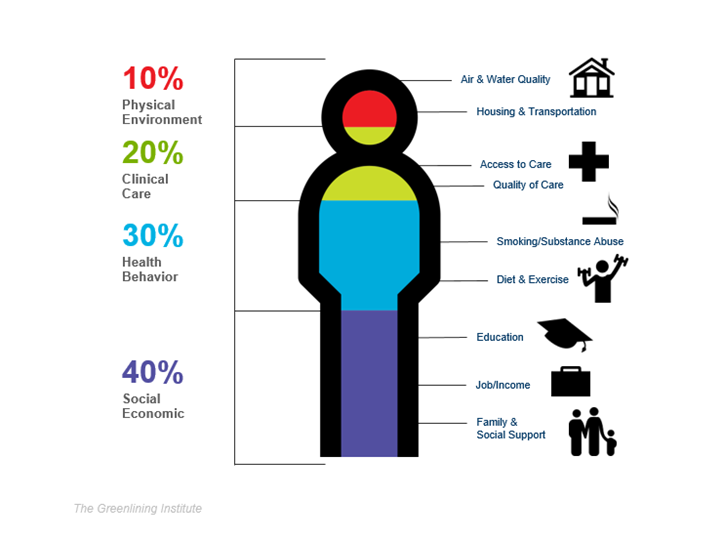
What are healthcare disparities? And what connection do they have to social well-being and overall health? Healthcare disparities refer to the higher health risks and the negative impact that certain groups have in comparison to others. According to the Green Lining Institute, social well-being contributes to 40% of one’s overall health. Social well-being is also attributed to one’s education level, job/income, and family/social support. An individual may appear physically and clinically healthy, and still not be “well” due to their socioeconomic status.
The COVID-19 impact on Black Americans has been significant. While data is still premature, we are seeing trends in states like Mississippi, where we see troubling disparities. Mississippi health officials have reported that 50% of COVID-19 related deaths are within the Black community – which only attributes to 30% of Mississippi’s population.1 This trend is not unique to Mississippi, in fact, 13% of the population in the states reporting racial/ethnic information, Black Americans account for about 34% of total Covid-19 deaths.”
These disparities are not necessarily about race. They are about the social inequities such as lack of access to good healthcare, nutritious food, and a healthy local economy. According to the U.S. Bureau of Labor Statistics, Black people are overrepresented compared to the overall population in the food service industry, hotel industry and taxi drivers and chauffeurs. These are “essential” jobs that typically offer less pay, minimal health insurance coverage and housing opportunities – which in a health crisis, puts them at a greater risk of contracting a disease and falling critically ill.

How can we address healthcare disparities before a crisis hits? First, we must understand the difference between health equality and health equity. Health equality means that everyone gets the same care, while health equity, according to the World Health Organization, implies that ideally everyone should have a fair opportunity to attain their full health potential and that no one should be disadvantaged from achieving this potential. See figures 1 and 2 below.
A good way to minimize health disparities is to understand what barriers that different communities are facing in order to achieve true health and wellness. Healthcare organizations such as AMN Healthcare recognize the impact that social inequities have on an individuals’ overall health and well-being. By having a commitment of Corporate Social Responsibility, internal programs that give people of color opportunities to achieve professional and personal development, such as SLIDE , an employee resource group focused on the professional and personal development for people of color. Externally, AMN Healthcare is proud to have a Business Diversity program which helps grow Small, Minority, Women, Veteran and LGBTQ owned businesses that impact the local economy.
Figure 1: Interactions Institute: http://interactioninstitute.org/illustrating-equality-vs-equity/

Figure 2: The Robert Wood Johnson Foundation further demonstrates the different between Health equality and Health equity.

References:
https://thehill.com/homenews/state-watch/491518-black-latino-communities-suffering-disproportionately-from-coronavirus
https://www.ksdk.com/article/news/health/coronavirus/st-louis-city-racial-data-covid-19-cases/63-f6a56b31-b744-4429-948b-d49cf50c3f57
https://www.amnhealthcare.com/diversity-equality-inclusion/
By: Maisam Ileiwi




