
Rise in Healthcare Overtime Threatens Patient Safety and Nurse Turnover
Healthcare workers are putting in more hours per week than ever before, according to newly released data, signaling potentially greater use of overtime in the face of continuing workforce shortages. This scenario creates many risks for healthcare organizations, because too much overtime has been linked to costly problems including medical errors and other threats to patient safety, declining patient satisfaction, clinician fatigue and burnout, depressed staff morale and rising turnover – and the bottom-line impacts from these problems.
The new data from the U.S. Bureau of Labor Statistics show that average weekly hours worked in all of healthcare and in hospitals in particular have reached record highs.
“The data infers that healthcare organizations may be using more overtime to cover for open shifts,” said Carolina Araya, Senior Vice President of Client Management at AMN Healthcare. “While this may seem like a viable option, a large and very convincing body of research shows that too much overtime can put a severe strain on nurses and other workers, which weakens their ability to provide quality patient care. Most clinicians will tell you plainly that this is true.”
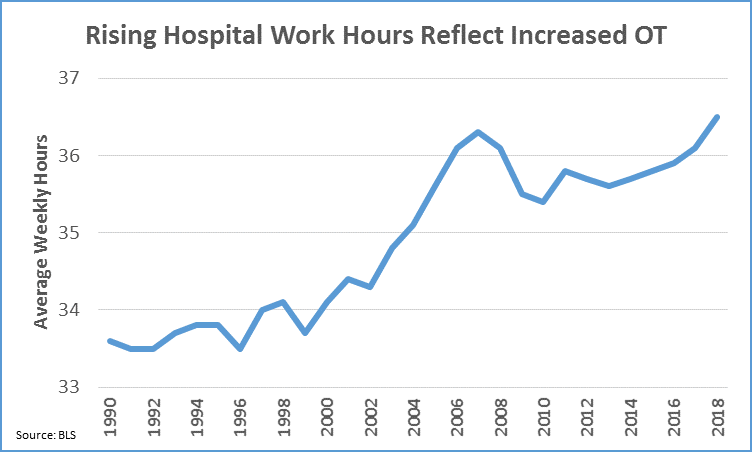 According to the BLS data, hospital industry employees reached 37.1 average weekly hours worked in February through June 2018. Meanwhile, healthcare sector employees as a whole hit 34 average weekly hours in April, May and 2018. The average weekly work hours represent both full-time and part-time, and the split between the two has remained steady. The weekly hours worked represent a record high for both categories dating back to 1990, when collection of these statistics began.
According to the BLS data, hospital industry employees reached 37.1 average weekly hours worked in February through June 2018. Meanwhile, healthcare sector employees as a whole hit 34 average weekly hours in April, May and 2018. The average weekly work hours represent both full-time and part-time, and the split between the two has remained steady. The weekly hours worked represent a record high for both categories dating back to 1990, when collection of these statistics began.
Nurse Fatigue and Patient Safety
Research (IOM, 2003) has linked fatigue to several types of performance issues that can compromise the patient care environment. These include a decline in short-term and working memory; a reduced ability to learn; a negative impact on critical thinking, innovation, and insight; increased risk-taking behavior; and impaired mood and communication skills. Most notably, healthcare worker fatigue has been tied to an increased risk of patient-care errors. Tired, sleep-deprived nurses are more prone to errors that can endanger patient safety.
This point is clearly illustrated in a groundbreaking study (Rogers et al., 2003) involving 393 nurses over more than 5,300 shifts. Researchers found that work duration, overtime, and number of weekly hours worked had significant effects on errors. Specifically, the likelihood of making an error in patient care was three times higher when nurses worked shifts lasting 12.5 hours or more. The error risk began to increase when shifts exceeded 8.5 hours.
The study was among those cited in a Sentinel Event Alert issued by The Joint Commission in 2011 and updated in May 2018. The Alert, Health Care Worker Fatigue and Patient Safety, which noted that “shift length and work schedules have a significant effect on health care providers’ quantity and quality of sleep and, consequently, on their job performance.” It recommended designing work schedules to minimize fatigue.
Nurse Burnout and Staff Turnover
Nurse burnout is an ongoing problem in the healthcare industry, and it increases costly staff turnover, according to several studies. A 2013 survey released by CareerBuilder showed that 60% of healthcare workers have experienced job burnout, with more than 20% saying they often or always feel burned out.
The CareerBuilder survey, conducted by Harris Interactive, found that 34 percent of the more than 500 U.S. healthcare workers surveyed plan to look for a new job this year. Among the reasons were long hours and juggling multiple patient needs.
 Nurses working shifts of ten hours or longer were up to two and a half times more likely than nurses working shorter shifts to experience burnout and job dissatisfaction and to intend to leave the job, according to a 2012 study of nurses working in 577 hospitals (Stimpfel et al., 2012). The study concluded that “extended shifts undermine nurses’ well-being, may result in expensive job turnover, and can negatively affect patient care.”
Nurses working shifts of ten hours or longer were up to two and a half times more likely than nurses working shorter shifts to experience burnout and job dissatisfaction and to intend to leave the job, according to a 2012 study of nurses working in 577 hospitals (Stimpfel et al., 2012). The study concluded that “extended shifts undermine nurses’ well-being, may result in expensive job turnover, and can negatively affect patient care.”
Also, the Nurse Staffing Strategy Survey, commissioned by Kronos Inc. for the American Organization of Nurse Executives (AONE) meeting in 2013, found that 69% of nurses said that fatigue had caused them to feel concern over their ability to perform during work hours. And 96% reported having felt tired at the start of their shift. Most respondents to the survey said that overtime is assigned more often than anticipated during a payroll cycle.
The desire to switch jobs was also evident in AMN Healthcare 2017 Survey of Registered Nurses. While a majority of nurses (60%) said they are satisfied with their current jobs, more than a third said they often feel like quitting, and they hope they will not be working at their current job in a year. Such numbers do not bode well for healthcare organizations. Hospital nurse turnover is on the rise; the average cost of turnover for a bedside RN is $49,500 and ranges from $38,000 to $61,100 (NSI Nursing Solutions, 2018).
Exploring Options to Overtime
Due to the high potential for negative impacts, healthcare organizations need to consider options other than overtime for ensuring appropriate nurse staffing levels.
A number of solutions exist:
- Create an optimal balance of permanent and contingent staff
- Improve float pool management
- Expand online staffing capacity
- Optimizing existing staff through workforce solutions
- Adopting technology-enabled forecasting of patient demand and staffing need
- Develop training programs to move new nursing graduates into practice
Expertise in healthcare staffing and workforce solutions resides outside the wall of the hospital today. Partnering with these external experts can help healthcare organizations reach and maintain staffing goals without risking patient care through too much overtime.
References
Institute of Medicine: Keeping patients safe: transforming the work environment of nurses. Washington, DC: National Academy Press, Nov. 3, 2003
Rogers A, Hwang W, Scott L, Aiken L, Dinges, D (2004). The Working Hours of Hospital Staff Nurses and Patient Safety. Health Affairs, 2004; 23(4):202-212
Stimpfel A, Sloane D, Aiken L (2012). The Longer the Shifts For Hospital Nurses, The Higher The Levels Of Burnout And Patient Dissatisfaction, Health Affairs, 2012 Nov; 31(11): 2501–2509.
2018 National Health Care Retention & RN Staffing Report (2018). NSI Nursing Solutions, Inc.
